oleh admin | Agu 25, 2025 | healthcare and medicine, illness, infectious diseases, news, public health
Released on, Aug. 19 – August 19, 2025 at 3:04 PM
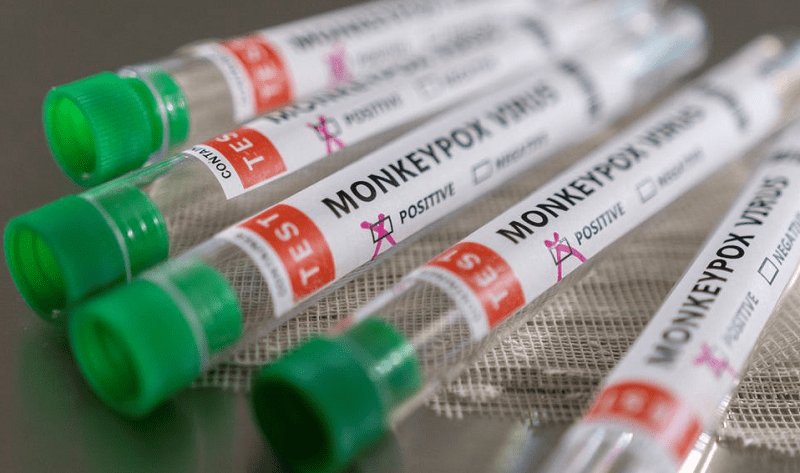
The first confirmed case at the Pakistan Institute of Medical Sciences (PIMS) in Attock was brought to Islamabad from Dubai on August 15, 2025, according to official reports.
Health officials mentioned that the individual showed signs of monkeypox when he arrived at the airport, leading basic health staff to immediately send him to the Pakistan Institute of Medical Sciences (PIMS) for additional assessment.
On August 18, the National Institutes of Health formally verified that the individual had been infected with monkeypox, and he is now undergoing home quarantine with medical oversight to avoid additional transmission.
Monkeypox is an uncommon virus that was first identified in monkeys and subsequently emerged in West Africa following the 1970s. In the past, the majority of infections were reported within Africa, although instances have also been recorded in Europe and the United States.
Specialists explained that monkeypox transmits through direct interaction and is less infectious than COVID-19. It can spread through damaged skin, airborne particles, or exposure to the eyes, nose, or mouth.
Common signs generally emerge between 7 and 14 days after exposure, featuring symptoms such as fever, head discomfort, joint soreness, tiredness, enlarged glands, and skin eruptions that often begin on the facial area before spreading throughout the body.
The virus may also spread via unguarded sexual activity, although not every individual acquires it in this manner. Officials recommend practicing physical separation and good sanitation to reduce the chances of getting infected.
oleh admin | Apr 19, 2025 | africa, health, health and healthcare economics, healthcare and medicine, public health
The leading public health organization in Africa intends to seek additional funding from local sources to safeguard the progress achieved in the last twenty years regarding disease outbreak readiness and management, due to a significant reduction in international assistance.
As official development assistance (ODA) for Africa has decreased by 70% in recent years, it has become evident that there is now a significant shortfall in healthcare financing. This situation is exacerbating the strain on vulnerable health systems.
Throughout history, Official Development Assistance (ODA) has played a crucial role in cutting the under-five mortality rate by half from 1990 to 2019. This assistance expanded access to routine vaccinations and bolstered HIV/AIDS prevention and treatment initiatives, which currently offer antiretroviral therapy to more than 18 million individuals throughout Africa. Additionally, ODA facilitated swift reactions during significant healthcare emergencies like the Ebola epidemic in Western Africa.
The reduction in funding parallels an upsurge in disease outbreaks. From 2022 to 2024, the continent experienced a 40% surge in recorded public health crises. There are ongoing worries regarding the resurgence of viral hemorrhagic diseases like Ebola and Marburg. Additionally, climatic disruptions—spanning everything from flooding to extreme heat—are generating fresh health threats, particularly in areas with limited capacity for response.
“Dr. Jean Kaseya, Director General of the Africa Centres for Disease Control and Prevention (Africa CDC), pointed out that we are grappling with several challenges related to managing debts and relying heavily on imported medical supplies. These combined issues pose a significant threat to Africa,” he stated.
This issue presents a larger challenge for Africa’s health security framework, yet efforts are underway to address the funding instability. The Africa CDC has encouraged African Union member states to embrace a fresh phase of healthcare investments. Dr. Kaseya suggests a tripartite approach aimed at boosting sustainability and decreasing dependence on outside funders, as detailed in her recent publication.
He is calling on African Union Member States to increase their domestic funding for public health. Only two countries currently meet the Abuja target of allocating 15% of national budgets to healthcare. Domestic commitment is essential to safeguarding health systems against the volatility of international funding, he notes. “We need to have a costed strategic plan and a national financing plan. We need to push for more alignment of external resources,” said Dr. Kaseya.
Secondly, the Africa CDC is seeking innovative financing strategies. This includes establishing the Africa Epidemics Fund, which debuted its operational framework in February 2025, serving as a consolidated asset for readiness against emergencies and swift responses. Additionally, the organization is investigating options like an aviation levy or collective solidarity taxes aimed at generating a consistent source of finance for managing disease outbreaks.
Thirdly, the Africa Centres for Disease Control and Prevention (Africa CDC) aims to strengthen partnerships with charitable organizations and businesses. This initiative seeks to secure sustained funding for vital infrastructures such as regional vaccine manufacturing facilities, digital healthcare platforms, and distribution channels. To achieve these goals, Africa CDC has introduced the African Pooled Procurement Service designed to reduce expenses and enhance availability of crucial medical supplies throughout the region.
In order to facilitate the mobilization of internal resources and explore innovative financial strategies, Africa CDC seeks an investment of $43 million. This sum will help implement their initiatives, ensuring significant advancements towards achieving lasting healthcare financing throughout the region.
“The document outlines a comprehensive budget plan for every area of support. This includes funding for technical aid in formulating costed national healthcare strategies, setting up an AU-managed tracking tool, executing the trial aviation levy, as well as crafting and expanding novel and mixed financial models,” states the report on health financing.
Stirring up wider backing, Dr. Kaseya spearheaded an important diplomatic delegation to the United States, Norway, and Denmark. During their visit to Washington, D.C., he and his team held meetings with US legislators, USAID representatives, officials from the US Centers for Disease Control and Prevention, as well as prominent charitable organizations such as the Bill & Melinda Gates Foundation and the Rockefeller Foundation. The purpose of these discussions was to underscore Africa CDC’s crucial position in ensuring worldwide health safety and to seek sustained assistance amid financial constraints faced by funding nations.
“Investing in public health in Africa is equivalent to investing in worldwide stability,” stated Dr. Kaseya during his trip to the United States. “The advancements made in Africa should not be undone due to short-term financial limitations faced by collaborating nations.”
According to Dr. Ngashi Ngongo, Principal Advisor to the Director General and the Continental Incident Manager for Mpox, what might appear as a significant obstacle could actually turn out to be a crucial chance.
“Africa CDC is utilizing reductions in international funding to promote sustainable healthcare financing — encouraging local investments, opening up new funding avenues, and constructing robust systems for Africa’s future,” states Dr. Ngongo.
Discussions held in Norway and Denmark with governmental and developmental authorities revealed a mutual desire to enhance healthcare infrastructure. Although concrete financial pledges remain pending, both nations expressed robust political backing for achieving the long-term goals of the Africa Centres for Disease Control and Prevention (Africa CDC).
While visiting Norway, Dr. Kaseya endorsed a fresh Memorandum of Understanding linking the Africa CDC with the Kingdom of Norway. This agreement zeroes in on bolstering capabilities, improving data utilization for informed decisions, and utilizing DHIS2—an open-source system designed for gathering, documenting, examining, and sharing both aggregated and individual-specific information—to support nationwide and cross-border illness monitoring efforts.
During these meetings, Dr. Kaseya stressed that Africa is looking for partnerships rather than charity. He stated, “Our request is for solidarity and joint investment.” According to him, what they are establishing serves as a barrier protecting both Africa and the globe.
Dr. Ngongo emphasizes that complaining won’t solve anything. He states, “Instead of just reacting, we must consider how to adapt proactively should this become the standard scenario—how can we stay competitive within these parameters? How do we implement necessary changes on our end so that we can transform current challenges into opportunities for Africa? Our approach has been focused on turning potential obstacles into chances for progress. For this reason, we’re implementing a fresh strategy—one that focuses on enhancing internal financial resources, exploring novel funding methods such as solidarity surcharges and excise duties, and attracting investments from the private sector. We view this not merely as a hurdle but also as an opportune time to redefine healthcare financing across the continent.”
The Africa Centres for Disease Control and Prevention (CDC) saw an enhancement in their funding efforts aimed at strengthening their capacity to respond to disease outbreaks and combat illnesses continent-wide. This advancement was supported by two African presidents on March 14.
On February 15, President João Manuel Gonçalves Lourenço of Angola assumed the leadership of the African Union (AU) during the inaugural ceremony for the 38th Ordinary Session of the AU Assembly of Heads of State and Government.
President Lourenço praised the significant achievements of the Africa CDC in promoting the continent’s public health goals, linking them closely with economic development and employment generation, as well as safeguarding the security and welfare of all African citizens.
He mentioned that Africa CDC is crucial for enhancing the continent’s ability to address new health risks swiftly and efficiently.
“The pivotal role this organization has undertaken has established an admirable benchmark in disease monitoring, prevention, and management, significantly enhancing both regional and international public health safety. I pledge ongoing and robust backing for Africa CDC, enabling you to effectively fulfill your crucial mission,” stated President Lourenço.
The Ethiopian Prime Minister, Abiy Ahmed, who likewise toured the Africa CDC during the same visit, urged AU member states to enhance their joint commitment towards bolstering the Africa CDC into a leading public health organization. “We must collectively fortify this entity alongside our partners,” stated Prime Minister Abiy Ahmed. He further appealed to other African leaders to unite in transforming the regional public health body into an exemplary institution dedicated entirely to improving healthcare throughout the continent.
Provided by Syndigate Media Inc. (
Syndigate.info
).

oleh admin | Mar 27, 2025 | health, healthcare and medicine, measles, news, public health
MANILA, Philippines – According to the Department of Health (DOH), they documented 1,185 instances of measles nationwide between January 1 and March 15. This figure represents an increase of “27% more” compared to the 930 cases logged over the identical timeframe in 2024.
In a Facebook update, the Department of Health reported that the regions with the most cases were: the National Capital Region with 295 instances; Central Luzon with 150 instances; and Calabarzon which includes Cavite, Laguna, Batangas, Rizal, and Quezon, totaling 144 cases.
READ:
68% of German measles cases in the Philippines are among those who are not vaccinated, according to the DOH.
The Department of Health cautioned parents to ensure their kids receive vaccinations for measles since out of all reported instances, 802 cases, which make up 68%, involved children who either did not get vaccinated at all or only received partial doses.
“If many children remain unvaccinated, it means the threat of measles is also increasing. That is why the DOH is once again urging parents to ensure their children receive the measles vaccine,” it added.
The agency stated that according to their immunization program, kids receive the initial vaccine dose at 9 months of age, followed by the second dose when they reach 12 months.
READ:
The Department of Health has vaccinated more than 640,000 children against measles.
Children between 13 and 59 months old who haven’t received all their vaccines can join a catch-up vaccination initiative.
The Department of Health earlier stated that vaccination is crucial to avoid complications like pneumonia, meningitis, and fatalities, particularly in children younger than five years old.

oleh admin | Mar 27, 2025 | coffee, food and drink, product recalls, public health, public health and safety
-
EXPLORE FURTHER: Critical alert released following significant coffee recall due to contamination issues
Many coffee items widely available throughout the Midwest and Great Lakes regions are subject to recall due to an issue with their labels.
A total of 692 decaffeinated product units are being removed from store shelves following tests that showed many containers actually held regular caffeinated coffee and were incorrectly labeled.
This might be hazardous to one’s well-being, since individuals with cardiac issues, hypertension, or those who are expecting are recommended to steer clear of caffeine due to possible adverse reactions.
Consuming a full-strength coffee
may cause
These individuals may experience palpitations, spikes in blood pressure, or various complications.
The
recall
Was started by Massimo Zanetti Beverage USA and includes 12-ounce packages of their Cherry-flavored Our Family decaffeinated ground coffee.
It was released in 15 states, including
Illinois
,
Michigan
,
Ohio
and
Wisconsin
, and impacts the lightly roasted variety with artificial flavoring.
If consumers own a recalled item, they haven’t been informed about the appropriate actions to take. Generally, this would involve discarding the product or getting a refund by returning it to the retailer.

The FDA initially disclosed the recall on March 12, and now the risk level of this issue has also been categorized.
This recall has been categorized as Level II, indicating that the products may pose some risks to specific individuals but are unlikely to lead to severe health issues.
Customers are advised to examine the rear portion of their Massimo Zanetti Beverage ‘decaf’ coffee containers to determine if they fall under the recall.
The recalled items have the UPC code 0 70253 11080 1 and are labeled with BEST BEFORE 080325 V 15:37 C’.
The states where the items were distributed include: Colorado, Iowa, Illinois, Indiana, Kansas, Kentucky, Michigan, Minnesota, North Carolina, North Dakota, Nebraska, Ohio, South Dakota, Wisconsin, and Wyoming.
The distribution was handled by the Michigan-based SpartanNash Company, and these items are marketed under the Our Family brand, widely recognized in the Midwest and Great Lakes areas.
The FDA cautions online: “Decaffeinated coffees and teas possess lower levels of caffeine compared to their standard versions, yet they still retain a small amount of caffeine.”
For instance, decaffeinated coffee usually contains between two to 15 milligrams in an 8-fluid-ounce serving.
‘If consuming caffeine leads to adverse effects for you, it might be best to steer clear of such drinks entirely.’
A typical cup of coffee has approximately 95 milligrams of caffeine.
Initially, all coffee contains caffeine. The decaffeination process involves immersing coffee beans either in water or a solvent to remove the caffeine content.
This could be due to the extraction of caffeine failing during processing at the facility, or because the coffee beans never underwent this procedure and were simply incorrectly labeled.
The symptoms of excessive coffee consumption can involve a heightened heartbeat, heart palpitations, sleeplessness, anxiety, tremors, stomach discomfort, or nausea.
Approximately 66 percent of Americans, which equates to about two-thirds, consume at least one cup of coffee daily.
Out of this group, approximately 10%, which equates to around 26 million individuals, reportedly consume decaf coffee every day.
Recently, this trend has gained traction due to the growing longevity movement, advocating reduced coffee intake to improve sleep quality. However, some individuals opt for decaf coffee for health benefits as well.
Read more

oleh admin | Mar 25, 2025 | infectious diseases, news, public health, viral diseases, viruses
-
EXPLORE FURTHER: Britain needs immediate action to combat fatal Disease X
Top health authorities have cautioned
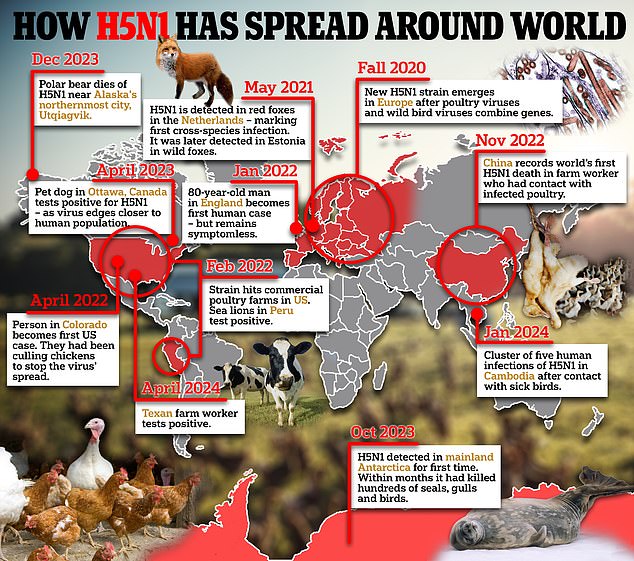
bird flu
might ignite the next pandemic, after a recent ‘development in the tale’.
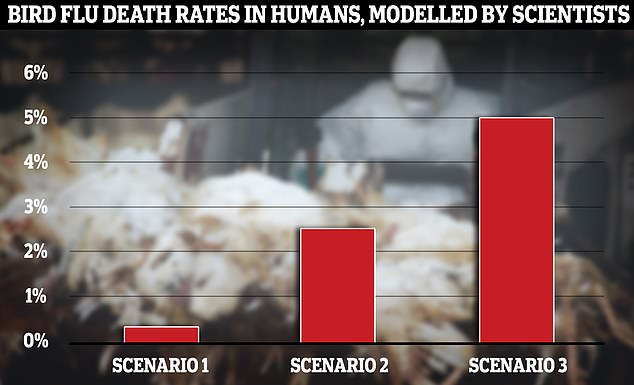
Richard Peobody, who leads the work on epidemic and emerging infections at The UK Health Security Agency, warned that the strain of the virus under scrutiny, H5N1, could potentially trigger a worldwide crisis akin to COVID-19.
He stated in Manchester today that ‘H5N1 has the capability to turn into a pandemic, potentially a future one.’
His remarks follow the detection of the virus in a sheep in Northern England yesterday.
the first known case
unique of its kind globally.
Regarding that transition across species, Mr Peabody mentioned it was a key aspect of how birds evolve.
flu
has undergone changes since it initially appeared in the 1990s.
As he mentioned, ‘Its characteristics have evolved over the last three or four years,’
We’re observing this phenomenon in the United States among dairy cows and various other animal species. Similarly, we’re noticing it here in the UK as well. Therefore, we are collaborating closely with our peers specializing in animal health to ensure that public health remains safeguarded.
When asked about whether UKHSA’s evaluation of avian influenza had shifted due to the latest incident, Mr. Peabody stated it introduced “a new turn in the narrative,” yet he also noted with relief that additional cases among sheep have not been detected.

He stated: “As usual, it enters this continuous, ongoing risk evaluation,” he explained. “Currently, that has not really altered.”
His remarks follow the UK Health Security Agency’s serious warning regarding 24 lethal viruses that have the potential to cause the next ‘Disease X,’ a term frequently used for the possible agent behind the future pandemic.
The body has narrowed the list down to four pathogens deemed to pose a significant pandemic threat, with bird flu being one of them.
The virus, exhibiting a worrying capability to leap across species, has already been identified in a single UK farmer who was reported to have come into contact with contaminated poultry.
In the meantime, the disease took its initial human life in the United States way back in January, resulting in the death of a 65-year-old individual with pre-existing medical issues after being exposed to their own group of wild birds.
A measles-like virus that could potentially be ‘significantly more hazardous than Covid’ has been added to the list, as per expert opinions.
A prominent scientist cautioned that the UKHSA list encompasses viruses which might prove ‘infeasible to contain with even the most rigorous measures.’
lockdown
’.
This prompted the government to unveil a new reference manual that will undergo constant updates, ensuring that scientists and researchers remain current regarding emerging risks.
One concerning pathogen belongs to the Picornaviridae family, known for causing viruses that lead to illnesses similar to polio.
For instance, consider the illness known as acute flaccid myelitis (AFM), a rare ailment that causes muscle weakness and paralysis.
In January, a 15-year-old lad from Rochdale ended up paralyzed following an AFM infection.
BBC
reported.
Health authorities have likewise cautioned that viruses from the Paramyxoviridae family could potentially lead to pandemics.
These encompass illnesses such as measles, mumps, and certain respiratory tract infections, along with the Nipah virus — known for transmitting from bats or pigs to humans — leading to encephalitis and fatalities.
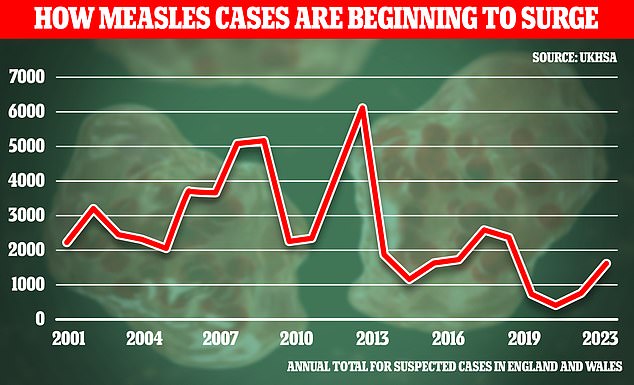
Significant measles outbreaks have already been documented globally due to falling immunization rates.
In last year, 2,911 instances of measles were confirmed in England, marking the highest annual tally recorded since 2012.
The severe disease, which predominantly impacts children, may lead to complications such as pneumonia, inflamed eyes and potential blindness along with swelling in the brain causing seizures, hearing impairment, and harm to the brain.

Other viruses that authorities are monitoring closely include coronaviruses like Covid-19 and
MERS, which has thus far claimed over 900 lives, predominantly in the Middle Eastern region.
Mark Woolhouse, who is a professor of infectious diseases at the University of Edinburgh, stated
The Mirror
Scientists are primarily worried about a virus similar to measles.
‘A virus similar to measles could present a much greater danger than COVID-19,’ he stated.
‘A such virus would possess a significantly higher reproduction rate compared to the initial strains of COVID, rendering it uncontrollable through even the most stringent lockdown measures.’
The R number indicates the average number of individuals that an infected person will transmit the virus to.
‘This is precisely the type of pandemic that global public health organizations worry about,’ he mentioned additionally.
Measles has demonstrated an ability to erase our immune memories, which suggests that a significant epidemic might lead to an increase in various other infections across the country.
According to a study conducted at Harvard Medical School in 2019, the measles virus can eliminate up to 75 percent of the antibodies that defend against various viruses or bacteria which a child had been previously protected from.
Dr Isabel Oliver, the Chief Scientific Officer for UKHSA, stated that the updated virus list serves as a means to showcase how scientific investigations can be directed towards enhancing the UK’s readiness against potential health risks.
‘We are employing this tool during our discussions with the scientific community to assist in directing investments towards areas that will yield the most significant outcomes.’
‘We trust this initiative will accelerate the development of vaccines and diagnostic tools precisely where they are critically required, ensuring we are thoroughly equipped for combating potential lethal pathogens.’
In September 2019, the now-disbanded Public Health England warned that growing bacterial resistance to antibiotics might contribute to what is known as Disease X.
Read more

oleh admin | Mar 25, 2025 | europe, infectious diseases, medicine and healthcare, news, public health
The measles outbreak in Romania persisted for almost three years until Dr. Claudia Cojocaru contracted the virus from a patient she treated in the infectious disease ward of a Bucharest hospital back in 2019.
The illness—one of the most highly infectious globally—struck her severely, even resulting in her admission to the very hospital where she was employed.
It was not until after Cojocaru made a recovery and gave birth to her second daughter nearly a year later that she came to understand how her illness would alter the course of her career. She transformed into an outspoken advocate for vaccinations in a nation plagued by widespread health misinformation, antiscience political tendencies, and a beleaguered healthcare sector.
“I got to know measles very intimately,” Cojocaru, a neonatologist who is also training in family medicine, told SANGGRALOKAHealth. “[Now] I’m the one [parents] call when they have mixed messages”.
Romania reports the lowest measles vaccination rate within the European Union, where only 62 percent of individuals were fully vaccinated as of 2023.
That’s well beneath the 95 percent threshold required to stop measles outbreaks among infants and individuals with compromised immune systems who can’t receive vaccinations.
The outcomes include further lethal outbreaks. Romania’s previous measles epidemic concluded in 2020, however, the government announced yet another one.
December 2023
.
Approximately 31,000 individuals were affected, resulting in 22 fatalities last year, with 44 percent of those cases being unvaccinated children under five years old. No particular cure exists for this condition.
However, even though Romania’s outbreak is the biggest one in Europe, it isn’t the sole nation dealing with measles.
In the last year, Italy, Germany, Belgium, Austria, and France have individually documented numerous cases, with infections continuing to rise.
expected to rise
in the coming months.
This suggests that Romania’s recent measles outbreak might serve as an early warning of similar epidemics that could occur in other parts of Europe.
“The challenge spans across the entire region,” Dr Dragan Jankovic, who heads up efforts towards measles elimination at the WHO’s European office, told SANGGRALOKAHealth.
2024 turned out to be the absolute worst year for measles in Europe.
since the 1990s
, he added. “This is precisely why nations must step up once more and begin vaccinating individuals who have yet to receive their shots.”
Why vaccination rates plummeted
By 2013, Romania’s measles vaccination rates were comparable to or exceeded those of numerous other European Union nations.
However, vaccinations declined during the 2010s because of an “uptick” in vaccine reluctance, postponements in immunisation schedules, kids dropping out of follow-up visits as their families relocated, insufficient vaccine supplies, and a significant exodus of medical professionals from the nation.
according to a study
headed by the country’s main public health institution.
“It’s akin to a perfectly mixed cocktail being prepared before an outbreak,” said Dr. Stefan Dascalu, an immunologist at Oxford University from Romania, who wasn’t part of the study, to SANGGRALOKA Health.
If you neglect one of these issues, it will spread.
The COVID-19 pandemic provided ample opportunity for such sentiments to flourish. Similar to what occurred in numerous other nations, false information about vaccines along with conspiracy theories resulted in widespread doubt towards public health measures, sparking an upsurge in anti-scientific discourse that aided in
raise three conservative political parties
to the Romanian parliament, where they currently have control over approximately
third of seats
.
“God has not been vaccinated,” Diana Sosoacă, the leader of the SOS Romania party, stated during a speech last year.
barred from running
In the latest presidential election, following a court ruling that found some of her remarks “at odds with democratic principles.”
Since the onset of the pandemic, public trust in standard childhood vaccinations has
plummeted
in Romania.
For Cojocaru and other vaccination supporters in Romania, combating online conspiracy theories and anti-scientific political stances is just part of the challenge. They must also confront healthcare professionals who oppose vaccines—sometimes even facing resistance from within the medical community itself.
Romania’s healthcare system lacks adequate resources; the nation allocates insufficient funds for its medical needs.
5.8 per cent
In terms of its Gross Domestic Product (GDP), it allocates approximately half of what the European Union spends on healthcare. The country continues to face challenges stemming from past corruption during the Communist period.
“You’ll still encounter this widespread belief that if I visit a doctor, I must offer a little bribe… as otherwise, they might not attend to my needs,” Dascalu explained.
Many people think doctors are “corrupt or earning substantial profits or influenced by pharmaceutical companies,” which is quite a complicated issue to tackle, he mentioned.
Moreover, the measles vaccine is provided at no cost and advised for young children, though it isn’t compulsory. Additionally, although medical students study the historical background of vaccines, they do not
always trained
On how to provide them to patients.
In the meantime, certain healthcare providers offer patients inaccurate details regarding vaccinations and their possible adverse reactions. Additionally, these professionals frequently fail to inform individuals about which vaccine corresponds to which illness or when they ought to come back for subsequent visits, as reported.
a 2019 study
those following vaccination discussions at clinics throughout Romania.
Officials from Romania’s National Institute of Public Health did not reply to SANGGRALOKAHealth’s queries for information.
When patients express worries or even conspiracy theories regarding vaccines, Cojocaru mentioned that she aims to remain composed and unbiased, clarifying that vaccinations such as the MMR (measles, mumps, and rubella) vaccine are among the most thoroughly researched and safest medications available.
Cojocaru also informs her patients that she has vaccinated her two children, aged 5 and 7, who are both healthy.
I avoid pushing or teasing them,” she stated. “I inform them that there’s no rush for making decisions; my channel remains open. Should they have questions or worries, they can reach out to me anytime.
Implications for Europe
Regardless of how many households Cojocaru convinces to get vaccinated, it won’t suffice if there remain clusters of unimmunized individuals since the illness spreads so easily.
In Romania’s previous measles outbreak, individuals lacking health insurance, people experiencing poverty, single-parent households, and the Roma ethnic group were notably more susceptible, as indicated by the national public health institute’s research.
However, “no individual nation can be immune to the introduction of the virus,” Jankovic stated. “Once this virus enters a country and comes into contact with susceptible individuals, it will lead to cases, and regrettably possibly even outbreaks.”
Only four European Union nations — Hungary, Malta, Portugal, and Slovakia — boast measles immunization rates at 95 percent or above.
In numerous nations, the number of susceptible individuals seems to be increasing. Since the pandemic began, routine childhood vaccination rates have declined globally, leading international health organizations to initiate a promotional drive known as the
“big catch-up”
in 2023.
Jankovic stated that typically, nations that performed well throughout the pandemic—such as those boasting robust healthcare systems, effective public health communication, and consistent approaches to managing the crisis—seem to be progressing smoothly with regular childhood vaccinations.
However, some nations with inadequately coordinated efforts, contradictory advice, and overburdened medical facilities now appear to be in a worse situation, he mentioned.
“If you experience confusion… this will inherently impact not just that particular vaccine, but also other vaccines already within the system,” Jankovic stated.
Experts warned that without a sustained effort to enhance trust in public health initiatives and increase vaccination rates for measles and other illnesses, similar issues facing Romania might emerge across other parts of Europe.
“We are now facing the danger of losing all these investments,” Jankovic stated. “Should those skeptical attitudes towards vaccinations turn into a worldwide trend, we will be in serious trouble.”











